Inflammatory Arthritis of the Hip
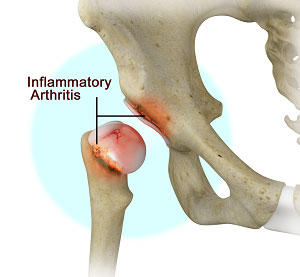
What is Inflammatory Arthritis of the Hip?
The inflammation of the joints is referred to as arthritis. Inflammation arises when the smooth lining called cartilage at the ends of bones wears away. In some cases, the inflammation is caused when the lining of the joint becomes inflamed as part of an underlying systemic disease. These conditions are referred to as inflammatory arthritis.
Types of Inflammatory Arthritis of the Hip
The most common types of inflammatory arthritic conditions of the hip include:
- Rheumatoid arthritis: Systemic disease of the immune system that commonly affects multiple joints on both sides of the body at the same time
- Ankylosing spondylitis: Chronic inflammatory disease of the spine and the sacroiliac joints (junction where the spine meets the pelvic bone)
- Systemic lupus erythematosus (SLE): An autoimmune disease in which the body’s immune system attacks its own healthy cells and tissues
Symptoms of Inflammatory Arthritis of the Hip
The typical symptom of arthritis is joint pain. Inflammatory hip arthritis is mainly characterized by an aching pain in the groin region, outer thighs or buttocks. The pain is commonly most severe in the morning and sometimes lessens with activity during the day. Vigorous activities may result in increased pain and stiffness, and limit your movement, making walking difficult.
Diagnosis of Inflammatory Arthritis of the Hip
Inflammatory hip arthritis can be diagnosed by a physical examination. Your doctor will ask you to move your hip in different directions to determine which motions are restricted or painful. X-rays and laboratory tests may be ordered to diagnose or rule out other conditions. X-rays may show thinning or erosion in the bones or loss in joint space. Laboratory studies will show the presence of a rheumatoid factor or other antibodies.
Treatments for Inflammatory Arthritis of the Hip
The treatment options vary depending on the diagnosis.
Non-surgical Treatment
Any infection in the hip joint is treated by non-surgical treatments that may provide relief with relatively few side effects.
- Anti-inflammatory medications or corticosteroids may help reduce the inflammation.
- Physical therapy may be recommended to help you increase the range of motion and strengthening exercises to maintain muscle tone.
- Assistive devices such as canes or walkers can make your daily living activities easier.
Surgical Treatment
Surgery is considered the last resort when the above non-surgical treatment options fail to reduce the symptoms. The type of surgery to be performed depends on your age, condition of the hip joint, and the type and progression of the inflammatory disease. The goal of surgery is to relieve pain and improve the joint motion. The most common surgical procedures include:
- Total hip replacement: Indicated for patients with rheumatoid arthritis and ankylosing spondylitis
- Bone grafts: Recommended for SLE. These grafts aim to build new blood cells to replace the old dead cells.
- Core decompression: Helps to reduce bone marrow pressure and encourages blood flow. Core decompression is another treatment option for SLE.
- Synovectomy: Removal of a part or whole of the joint lining. This is indicated if the inflammation has not affected the cartilage, but is limited to the joint lining or synovium.
Related Topics
- Hip Dislocation
- Leg Length Discrepancy
- Hip Fracture
- Pelvic Fractures
- Acetabular Fracture
- Femur Fracture
- Bisphosphonate Related Fracture
- Distal Femur Fracture
- Osteoarthritis of the Hip
- Inflammatory Arthritis of the Hip
- Hip Pain
- Stress Fractures of the Hip
- Femoral Neck Fracture
- Femoral Shaft Fracture
- Hip Instability
- Subtrochanteric Hip Fracture
- Periprosthetic Hip Infection





